
What is POTS disease?
The full form of POTS is postural orthostatic tachycardia syndrome.
POTS is a blood circulation disorder caused by two factors:
A particular group of symptoms typically happen when standing upright.
A heart rate increase of at least 30 beats per minute in adult people, or at least 40 beats per minute in teenagers, recorded within the first 10 minutes of standing (or as tested on a tilt table).
POTS impacts a range of individuals but is most common in women and girls aged 15-50 years old. While some people only experience minor symptoms, others feel that the disorder has an impact on their quality of life. POTS frequently get better gradually over time, & there are a few medications & self-care measures that may help.
What occurs in POTS?
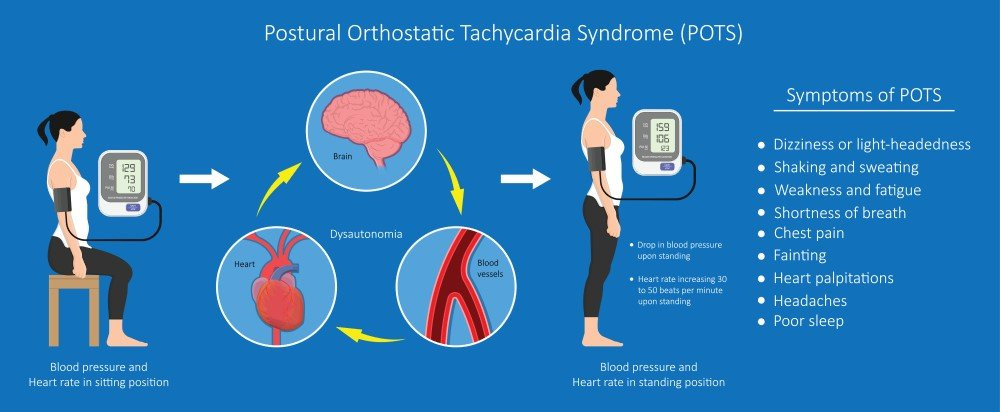
Commonly when you stand or sit up, gravity pulls some of your blood down to your hand, feet, and belly area. The autonomic nervous system, which is the neural system in charge of automatic body functions, accomplishes all of this without the need for conscious thought. The autonomic nervous system doesn't work correctly in POTS. There is a drop in blood supply to the brain and heart when you become upright & your heart races to compensate for it.
Treatment for POTS.
Postural orthostatic tachycardia syndrome treatment should be tailored to each person because the symptoms & underlying conditions can vary widely. Although POTS does not have a recognized cure, most individuals can control their condition with exercise, diet, and medication.
POTS diet
Throughout the day, drinking plenty of fluids is the cornerstone of treating POTS. The target is at least 64–80 ounces (about 2-2.5 liters) per day for the majority of POTS patients. Additionally, you would have to consume more salty meals and supplement your diet with salt shakers or salt pills.
These dietary modifications help keep water in your bloodstream, allowing more blood to reach the brain and the heart. Some patients' POTS symptoms may worsen when they consume particular foods or beverages. For instance, alcohol almost always makes POTS worse.
It diverts our body's blood away from the central circulation to the skin & raises the loss of fluids via urine. Caffeine might make a few people more lightheaded & nervous, but for some, it may help improve the tightness of blood vessels.
Your regular doctor or a POTS expert can assist you in determining how your food and particular medications can be helping or interfering with your treatment.
Postural Orthostatic Tachycardia Syndrome Exercise
Some POTS sufferers get relief from physical therapy. Physical treatment needs to start off slowly and increase based on your tolerance rather than following a set schedule because POTS symptoms can occasionally get worse with activity.
Exercise intensity may be gradually raised when your blood circulation improves as a result of your diet and prescription drugs. The motive is to retrain the autonomic nervous system to enable more exercise, which helps boost blood volume.
Those who are unable to stand up straight can begin exercising while lying down or in a reclining position. Aquatic therapy can be effective for a few POTS patients because water creates pressure around the system.
Many professionals find that manual physical therapy that addresses problems with nerve tightness & range of motion acts as a bridge to make better tolerance of exercise.
Medication for POTS
While no single medicine is helpful for everyone with POTS, most individuals with frequent symptoms impacting their quality of life require some form of medicine. The search for the correct medication or mixture of drugs needs patients & persistence on the part of both patients & doctors.
These drugs might focus on the following:
- Increasing blood flow
- lowering heart rate or helping to block the impact of adrenal hormones on the heart (for example, beta-blockers)
- maintaining sodium in the kidneys (e.g., fludrocortisone)
- Improving blood vessel constriction (e.g., midodrine)
Other treatments for POTS
- You may wear compression garments; it would help decrease excessive blood pooling in your legs. Besides, some specific postures while sleeping or sitting might also help decrease POTS symptoms.
- Avoid consuming a lot of caffeine or alcohol and slowly get up from a lying position.
- Include additional salt in your diet, but consult a physician first if you have high BP (blood pressure), kidney illness, or a heart condition, as it is not recommended.
Is POTS a severe condition?
POTS is not a life-threatening condition, but it can change your life. Falls caused by fainting is one of the main concerns for patients with POTS. People with POTS do not always faint. It might be an uncommon or rare event for those with fainting problems.
Symptoms of having POTS disease.
POTS can start gradually or unexpectedly in some people. Occasionally, you may have symptoms right away or a few minutes after standing or sitting up. Some of the symptoms might go away if you lie down.
Typical POTS symptoms include:
- Fainting, light-headedness, or dizziness
- Sweating and shaking, headaches, poor sleep
- Shortness of breath, chest pain, headaches, feeling sick
- Tiredness and weakness
- Problems with memory, thinking & concentration
Some individuals notice that feeling hot, engaging in strenuous exercise, eating, or having a period might worsen their symptoms.
Pregnancy and POTS
A frequent query is if POTS will impact pregnancy because it affects women of childbearing age. Usually, more than half of pregnant women with POTS reported feeling better than usual during their pregnancies may be due to the increase in blood volume present after the initial few weeks of pregnancy.
Others experienced a more variable course, with either stable symptoms of POTS or an increase in its symptoms. Other pregnancy complications appear to occur with about the same frequency in women with POTS, and their newborn babies seem to be as healthy as infants born to mothers without postural orthostatic tachycardia syndrome (POTS).
Can POTS (postural orthostatic tachycardia syndrome) go away?
POTS symptoms can gradually improve or go away over time. They might return just as surprising. The lack of symptoms doesn't mean that the cause of POTS is gone as well.
Who can treat POTS (postural orthostatic tachycardia syndrome)?
Your primary care physician is frequently qualified to treat POTS. It is often beneficial to get advice from a neurologist or cardiologist with knowledge of POTS for complex POTS situations. Physicians specializing in rehabilitation may also help you develop an exercise plan that can be helpful for you and work for treating POTS.















Leave a Reply